Introduction: Translating Healthcare into Data
Modern healthcare runs on data.
Every hospital admission, diagnosis, surgical procedure, prescription, and laboratory result generates information that must be recorded, interpreted, and analyzed. But the healthcare system cannot function efficiently using only free-text clinical notes written by physicians.
Instead, healthcare relies on standardized classification systems that convert medical documentation into structured data.
This process is known as healthcare coding.
Two terms frequently appear in this field:
- Medical Coding
- Clinical Coding
For many newcomers—especially in India—the difference between these terms can be confusing.
Training institutes often present them as two separate careers, while international health systems sometimes use them interchangeably.
The reality is more nuanced.
In most countries around the world, including Australia, Canada, and the United Kingdom, the profession is officially called Clinical Coding, and it includes the same responsibilities that the United States calls Medical Coding.
However, in insurance-driven healthcare systems like the United States, the term Medical Coding is strongly linked with billing, reimbursement, and Revenue Cycle Management (RCM).
Meanwhile, Clinical Coding is sometimes associated with health statistics, epidemiology, and hospital data analysis.
Understanding this global distinction is essential for Indian professionals entering the international healthcare coding market.
In this comprehensive guide, we will explore:
- The real difference between medical coding and clinical coding
- How coding supports hospital funding through Diagnosis Related Groups (DRGs)
- The roles of Health Information Management (HIM) and Revenue Cycle Management (RCM)
- Global coding standards used in USA, UK, UAE, and Saudi Arabia
- Specialized coding systems such as MedDRA used in clinical research
- The future of coding in the era of AI and digital healthcare
By the end of this guide, you will have a complete global understanding of healthcare coding as a profession.
Understanding the Core Concept: Healthcare Coding
Healthcare coding is the process of analyzing clinical documentation and assigning standardized alphanumeric codes that represent diagnoses, procedures, and healthcare services.
These codes allow healthcare systems to:
- Process insurance claims
- track disease patterns
- monitor hospital performance
- conduct clinical research
- plan national healthcare resources
Without coding, healthcare data would remain unstructured and impossible to analyze at scale.
A coder therefore acts as a translator between clinical medicine and healthcare data systems.
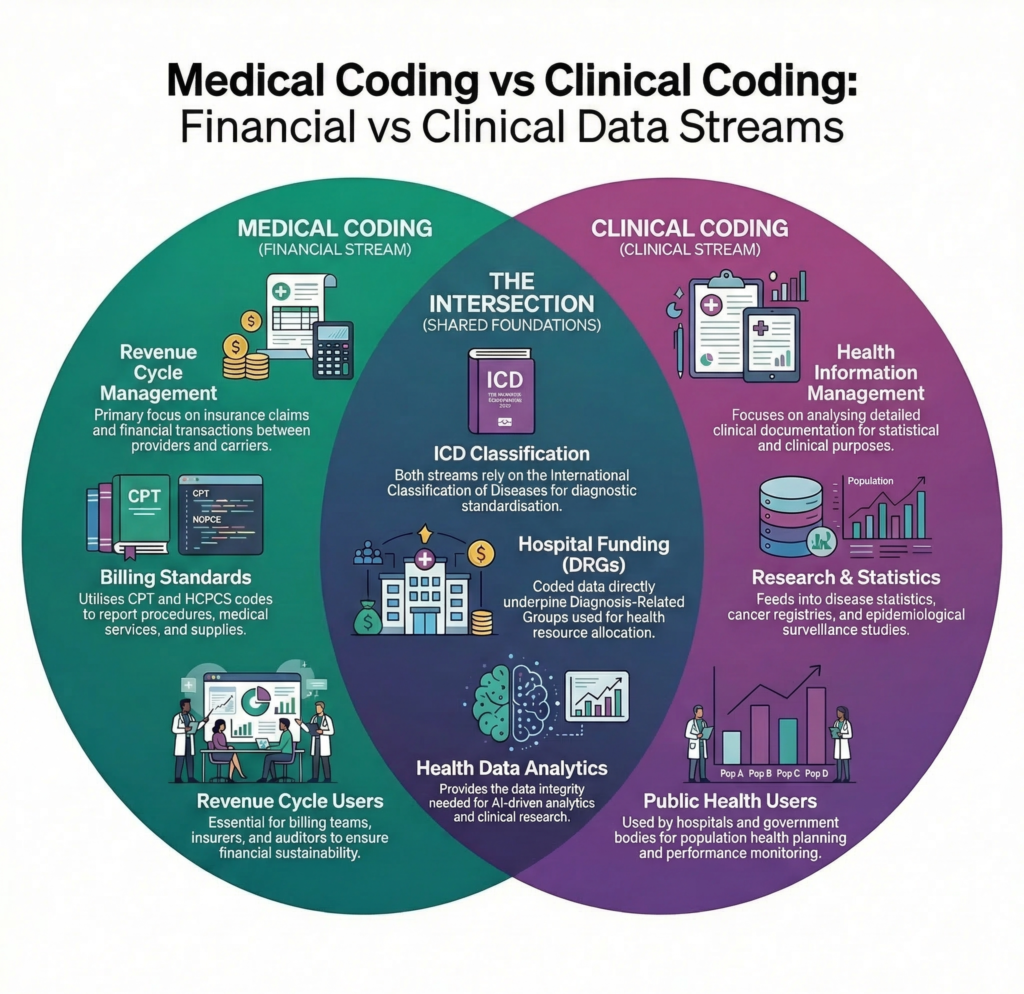
Medical Coding vs Clinical Coding: The Global Reality
The biggest misconception in this field is that medical coding and clinical coding are always different professions.
In reality, the difference is mostly terminological and regional.
Countries Where Both Terms Mean the Same
In many healthcare systems, Clinical Coding is simply the official job title for medical coding professionals.
Examples include:
- Australia
- United Kingdom
- Canada
- New Zealand
- Ireland
In these countries, clinical coders:
- analyze medical records
- assign diagnosis and procedure codes
- ensure accuracy of hospital data
- support funding models such as DRGs
This is essentially the same work performed by medical coders in the United States.
Countries Where Terminology Differentiation Exists
In US-influenced healthcare systems, the terminology evolved differently.
Here the profession is commonly described as Medical Coding because it is tightly connected with:
- insurance claims
- reimbursement
- revenue cycle management
- regulatory compliance
Meanwhile, Clinical Coding may be used more broadly in health statistics, registries, or research environments.
Key Differences (Conceptual Perspective)
| Aspect | Medical Coding | Clinical Coding |
|---|---|---|
| Primary Context | Revenue Cycle Management (RCM) | Health Information Management (HIM) |
| Core Objective | Insurance claims & reimbursement | Clinical data reporting & statistics |
| Main Users | Billing teams, insurance payers | Governments, researchers, registries |
| Typical Code Sets | ICD-10-CM, CPT, HCPCS | ICD-10, SNOMED CT, ICD-O |
| Focus | Financial accuracy | Clinical data integrity |
However, in countries like Australia, the clinical coder performs both functions.
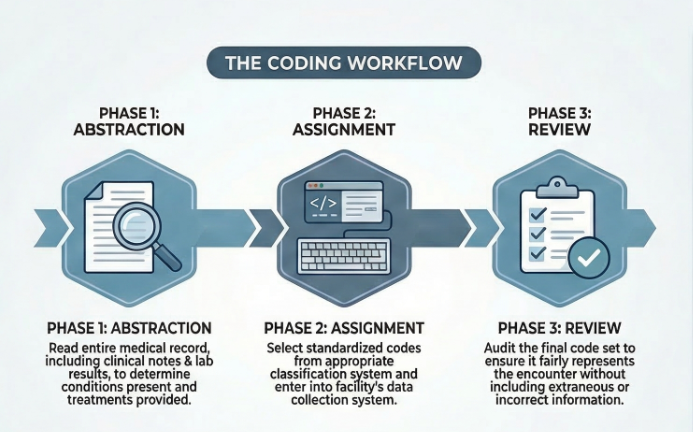
The Healthcare Coding Workflow
Regardless of terminology, coding follows a standardized professional workflow.
1. Abstraction
The coder reviews the entire medical record including:
- physician documentation
- operative notes
- laboratory reports
- radiology reports
- discharge summaries
The goal is to identify all relevant diagnoses and procedures.
2. Code Assignment
Codes are selected from classification systems such as:
- ICD
- CPT
- HCPCS
- SNOMED CT
3. Validation
The coder verifies that the codes:
- accurately represent the patient encounter
- follow coding guidelines
- support medical necessity
4. Data Integration
The coded data is then used for:
- insurance claims
- hospital reporting
- national healthcare statistics
Hospital Departments Connected to Coding
Coding does not exist in isolation.
It is integrated into the broader hospital administrative structure.
Two major organizational frameworks influence coding:
Health Information Management (HIM)
HIM focuses on clinical data governance.
Responsibilities include:
- medical record management
- coding accuracy
- data privacy compliance
- health statistics reporting
Clinical coders usually work within HIM departments in countries with national health systems.
Revenue Cycle Management (RCM)
RCM focuses on the financial lifecycle of a patient encounter.
It includes:
- Patient registration
- Insurance verification
- Clinical documentation
- Coding
- Billing
- Claims submission
- Payment collection
In US-style systems, coders operate inside the mid-cycle stage of RCM.
Clinical Documentation Improvement (CDI)
CDI teams bridge the gap between clinicians and coders.
They ensure physician documentation contains sufficient detail.
Example:
Instead of:
Pneumonia
CDI requests clarification:
- bacterial pneumonia
- viral pneumonia
- aspiration pneumonia
Better documentation leads to more accurate coding and reimbursement.
DRGs: The Financial Engine of Hospitals
One of the most important concepts in hospital coding is Diagnosis Related Groups (DRGs).
A DRG is a classification system that groups hospital cases based on:
- diagnosis
- procedures
- patient age
- complications
- severity of illness
Instead of billing every individual service separately, hospitals receive a fixed payment for the DRG category.
Example
Two patients with pneumonia may receive different DRGs:
Simple Pneumonia → lower payment
Pneumonia with complications → higher payment
The assigned DRG depends on the codes submitted by the coder.
Incorrect coding can therefore result in:
- underpayment
- compliance issues
- audit risk
This is why coding accuracy directly affects hospital financial sustainability.
Benefit Packages and Medical Necessity
Insurance companies use coding to determine whether services are covered under a patient’s benefit package.
For example:
A knee MRI may only be approved if the diagnosis code indicates:
- ligament injury
- severe trauma
- chronic knee instability
If the diagnosis code does not justify the procedure, the claim may be denied.
Coders therefore play a key role in demonstrating medical necessity.
Global Coding Systems: Country-by-Country
For Indian professionals working in international healthcare outsourcing, understanding global coding systems is critical.
United States Coding System
The US has the most complex coding environment.
Diagnosis Codes
ICD-10-CM
Over 70,000 diagnosis codes used for diseases and conditions.
Inpatient Procedure Codes
ICD-10-PCS
More than 75,000 procedure codes used by hospitals.
Physician Procedure Codes
CPT (Current Procedural Terminology)
Used for outpatient procedures and physician services.
Supply and Equipment Codes
HCPCS Level II
Used for:
- medical devices
- injectable drugs
- ambulance services
United Kingdom Coding System
The UK uses the term Clinical Coding within the National Health Service (NHS).
Diagnosis Codes
ICD-10
Procedure Codes
OPCS-4
Professional certification includes the National Clinical Coding Qualification (NCCQ).
United Arab Emirates Coding System
The UAE healthcare sector uses US-style coding systems.
Common standards include:
- ICD-10-CM
- CPT
Coders must often pass licensing exams from:
- DHA (Dubai Health Authority)
- DOH / HAAD (Abu Dhabi)
- MOH (Ministry of Health)
Saudi Arabia Coding System
Saudi Arabia uses coding standards influenced by Australia.
Diagnosis classification includes:
- ICD-10
- ICD-10-AM
Coders may need to pass the SCFHS Prometric exam for licensing.
Specialized Coding Systems in Research
Beyond hospital coding, specialized classification systems exist.
MedDRA (Medical Dictionary for Regulatory Activities)
MedDRA is used in:
- pharmaceutical companies
- clinical trials
- drug safety monitoring
It standardizes the reporting of adverse drug reactions worldwide.
ICD-O
Used in cancer registries to classify:
- tumor location
- tumor morphology
Artificial Intelligence and Coding
AI technologies such as Natural Language Processing (NLP) are increasingly used to assist coders.
Automated systems can:
- scan medical records
- suggest potential codes
- identify missing documentation
However, AI still struggles with:
- clinical context
- ambiguous documentation
- complex coding rules
Human expertise remains essential.
Why India is Becoming the Global Coding Hub
India has become a major center for healthcare coding services.
Reasons include:
Large life-science graduate workforce
English language proficiency
Cost-efficient outsourcing model
Growing healthcare IT industry
Many Indian coders work remotely for:
- US hospitals
- insurance companies
- healthcare analytics firms
- clinical research organizations
FAQ: Medical Coding vs Clinical Coding
Is medical coding different from clinical coding?
In most countries they are the same profession.
However, in the US the term medical coding is commonly used in billing and revenue cycle management.
Is clinical coding the same as medical coding in Australia?
Yes. In Australia the profession is officially called clinical coding, and it includes the same responsibilities performed by medical coders in other countries.
What is a DRG?
A Diagnosis Related Group is a system that categorizes hospital cases to determine reimbursement based on clinical complexity and resource usage.
Do I need a medical degree to become a coder?
No. Most coders enter the profession through specialized training programs in anatomy, medical terminology, and coding standards.
Which certification is best for Indian coders?
Popular certifications include:
- CPC (AAPC)
- CCS (AHIMA)
These certifications are widely recognized globally.
Final Thoughts
Medical coding and clinical coding form the data infrastructure of modern healthcare systems.
While terminology varies across countries, the core mission remains the same:
Transforming complex medical documentation into structured data that powers healthcare operations.
From hospital funding through DRGs to global disease surveillance and pharmaceutical research, coding professionals ensure that healthcare systems can understand and act on medical information.
For Indian professionals entering this field, mastering global coding standards offers a pathway to international careers in one of healthcare’s most data-driven professions.